1:30min
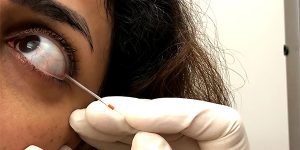
Photo courtesy UNSW Sydney
By Helen Carter
Journalist
Optometrists may soon be able to extend their scope of practice by using a tear sample to screen for early diabetic peripheral neuropathy in patients.
New research from UNSW Sydney published this week in The Ocular Surface is the first to show that peripheral nerve damage in type 1 diabetes can be traced in tear film.
Senior lecturer and postgraduate research co-ordinator in the School of Optometry and Vision Science, UNSW Sydney, and deputy editor of Optometry Australia’s Clinical and Experimental Optometry Dr Maria Markoulli is the senior author of the study. The lead author is Indian optometrist Mr Shyam Sunder Tummanapalli who is studying his PhD at the School of Optometry and Vision Science, and Director of Research in the school, medical microbiologist Professor Mark Willcox is also on the research team.
‘We found that people with type 1 diabetic peripheral neuropathy – which can result in recurring ulcers of the feet and in severe cases require amputation – have significantly reduced levels of a protein known as ‘substance P’ in their tear film,’ Dr Markoulli said.
‘About 119,000 Australians have type 1 diabetes. In the future, they may be able to have a quick tear sample collected either at their optometrists, the chemist, GP or endocrinologist, and be told whether they are at risk.’
Nerve damage cannot be reversed but early detection can help patients better manage the condition and prevent further complications, however existing early testing options are limited to invasive examinations including skin biopsies.
‘Peripheral neuropathy is notoriously difficult to detect early on and requires specialty training,’ Dr Markoulli said. ‘Our method would be done quickly, non-invasively and potentially by a non-specialist.
‘We would anticipate a screening tool could detect those at risk and show early signs of neuropathy, and these patients could then be referred for more confirmatory tests and management.
‘The idea is a point-of-care-device could be developed for optometrists, doctors and chemists to have in their practice/workplace to take a tear sample on the spot to detect early stage neuropathy.’
The research was a collaboration with the Prince of Wales Hospital and the team included researchers with expertise in vision science, diabetes, endocrinology, neurology and exercise physiology.

UNSW Sydney researchers on the team, L-R, Dr Maria Markoulli, Mr Shyam Sunder Tummanapalli and Professor Mark Willcox
Dr Markoulli said the idea for the study began when previous research from other groups including those led by Professor Nathan Efron from QUT discovered there were less corneal nerves in diabetic neuropathy. The team at UNSW then hypothesised that this would also result in a depletion in the levels of various substances by these nerves into the tears.
The UNSW team then tested the concentration of two proteins or neuropeptides in the tear film of 38 people with type 1 diabetes, 25 people with type 2 diabetes and 63 healthy age-matched controls because tear film can deteriorate with age. Photos of corneal nerves were also taken.
The researchers found that patients with type 1 diabetes and neuropathy had significantly less ‘substance P’ in tears than people without neuropathy and healthy controls.
They also found that the more severe the neuropathy, the less substance P the people with type 1 diabetes had.
‘People with type 2 diabetes and neuropathy didn’t have reduced levels of substance P, possibly because people with type 2 are generally older and may have depleted levels because of age,’ Dr Markoulli said.
‘This may also be perhaps because these two types of diabetes have different pathologies and risk factors,’ Mr Tummanapalli wrote.
Dr Markoulli said it also told researchers that the two disease processes were quite different.
Further study is required before tear testing becomes available clinically and the researchers hope to study ‘substance P’ loss over time according to varying severities of peripheral neuropathy.
The team will study more proteins in the tear film of those with type 1 and type 2 diabetes to get a fuller picture, and expand the study to determine specific changes in type 2 diabetes, trying to understand why these patients do not have the same biomarkers, what proteins change and if there is also a link to the tear film and peripheral neuropathy in type 2.
Peripheral neuropathy is the most common complication of diabetes and affects nearly half of all diabetes patients. It occurs when chronically high blood sugar damages the nerves connecting the brain and spinal cord to the rest of the body.
Symptoms include pain, numbness, imbalance, weakness, pins and needles, and recurring foot ulcers.
Tagged as: Diabetes, Future, Patient management, Practice equipment, Scope of practice, Universities