Optometry WA Resources
Optometry WA resource information and updates you need to know from your OWA Office. Click on the above blue Tabs to navigate on the Resources Section.
The Membership Tab contains current information on membership renewals.
The Referrals Tab will give you the option to go to our most recent page, Referral Updates – LISTS UPDATED JULY 2024
Driving Tab – New for 2022 – This contains the changes for Assessing Fitness to drive & all health professionals conducting fitness to drive assessments and providing advice to drivers will also be expected to refer to the new edition.
If you have any queries, please email admin@optometrywa.org.au
<< Back to Optometry WA home To Optometry WA – Our events >>

Optometry WA Membership Renewals
Renewals due by 30th June 2024 –
Memberships run from 1st July 2024 to 30th June 2025.
Recent Graduate Membership is available for 1 year’s discounted membership only, following on from our 6 months free Immediate Graduate Membership. Immediate Graduate Memberships running from 1st July 2024 to 31st December 2024 will benefit from our 6 months free membership and will need to renew at the end of this year.
We also have the new Career Break membership category for those taking a min of 6 months off from the optometry industry. Contact the OWA Office for further information. 9321 2300 or email as below.
Any membership queries, please email admin@optometrywa.org.au

Optometry WA Hospital Referrals
Optometry WA has compiled documents to assist OWA members with the referral procedures to the hospitals in Perth. The information has expanded and can be found on its own page here (member access only); Updated March 2022.

Fitness to Drive Summary of Changes
ASSESSING FITNESS TO DRIVE 2022
From 22nd June 2022 all licensing decisions made in relation to medical conditions and disabilities will be made using these standards.
Health professionals conducting fitness to drive assessments and providing advice to drivers will also be expected to refer to the new edition.
The redeveloped Austroads website is also now live, offering ready access to the new standards and practical information to support health professionals, drivers and industry. The user-friendly searchable html format includes alerts to highlight the recent changes to the standards as well as links to consumer information.
There is also an opportunity for health professionals, consumers and other stakeholders to subscribe to our regular updates. These will be published quarterly, providing information about fitness to drive issues and initiatives.
Changes or clarification on the following:
- Visual Fields (updated criteria)
- Monocular Vision (updated criteria)
- Visual Acuity (no criteria changes – clarification)
- Diplopia (no criteria changes – clarification)
- Telescopic Lenses (bioptics) (no criteria change)
- Updated driver medical standards – now available via the Austroads website
- All health assessments conducted for the purpose of establishing fitness to drive must be conducted according to the new edition.

Optometry WA Locum List
Locum list here in WA for those that want to work metro, regional or interstate.
Want to join the Locum List?
Please register yourself here by completing this short online form. Your information will then be made available to those that request access to the OWA Locum List. You will be required to update / confirm your continued presence on the list from time to time. If you have any queries, please contact the OWA office on admin@optometrywa.org.au
Want to access the Locum List?
Please email admin@optometrywa.org.au to request a copy of the list be emailed to you. You must be an optometrist practice and adhere to our t&c’s for using the list.
Want to become a Locum?
There are some very helpful documents already available on this Optometry Australia website – Click here to go to the Career & Employment Section / Working as a Locum The guides contain very similar information state to state and therefore there is currently no WA guide as the information you require is here. If you are in WA and need assistance with an aspect particular to WA, then please contact admin@optometrywa.org.au


Donations Gratefully Received
Here at Optometry WA we collect your old unwanted spectacles, sunglasses and cases and recycle them so they can be used again. Spectacles are new or old, are used in our St Pat’s Homeless Eye Clinic and the annual City of Perth Homeless Connect. The remainder go to the Acacia Prison for recycling in their dedicated, in house facility and then on to charities within Australia, as well as overseas aid.
Sunglasses (non prescription) and cases are just as important as frames and are greatly appreciated by those at St Pat’s and Homeless Connect. We also gladly accept donations of new frames and cases, just contact the OWA office to arrange a delivery time to the West Perth or a collection if is metro Perth.
If you would like to set up a collection box in your practice, please contact the OWA office on admin@optometrywa.org.au

WA Vacanation / Mask Mandate Update & Isolation Update - November 2022
For the latest information sent out from the OWA Office direct to OWA Members, you can view COVID-19 related emails here containing information for our OWA Members.
COVID REGS UPDATE: FRIDAY 4th NOVEMBER
Latest update advised to the OWA Office today direct from the CHO WA: Masks and Vaccinations no longer required for members in WA as of 12.01am Friday 4 November
The Honourable Mark McGowan, MLA, Premier of Western Australia announced this morning that the COVID-19 State of Emergency will end at 12.01am this Friday 4 November.
At that time, the Directions issued under the Emergency Management Act 2005 and Public Health Act 2016, including the COVID Transition (Face Covering) Directions (No 10) and Primary Healthcare Worker (Restrictions on Access) Directions ( Vaccination mandate) will fall away.
This will mean that there will be no mandatory face mask or vaccination requirements in WA from that time, though healthcare facilities and businesses may implement their own health and safety policies should they choose to.
No Longer Mandated Nov 2022
Latest update advised to the OWA Office today direct from the CHO WA: Masks and Vaccinations no longer required for members in WA as of 12.01am Friday 4 November 2022.
Optometry WA and the Reconciliation Action Plan
Optometry WA and the Reconciliation Action Plan process:
We acknowledge the traditional custodians of the land in which we live and work on here in WA, we pay our respects to their Elders past, present and emerging.
This is statement (or similar) often heard and repeated but, stated without understanding and sincerity, it is worthless.
We have a strong history in OWA of engaging with and providing services for the Aboriginal and Torres Strait Islander communities. Individual optometrists also do so through the Visiting Optometrist Scheme (VOS) run by Rural Health West for the Commonwealth Department of Health and through outreach services from or in our own practices.
The board of Optometry WA has agreed to explore a Reconciliation Action Plan (RAP) to become more inclusive and supportive of our Aboriginal communities. We understand that it will take generations for true healing and acceptance to occur. It is our belief that all people and communities in WA will benefit from a process of cultural awareness, acceptance of the past, awareness of present unconscious bias and racism and a mutual path forward for better futures.
To this end Optometry WA has formed a committee to investigate the Reconciliation Action Plan (RAP) process and we hope to bring along as many practitioners, staff and family with us as feel comfortable with the journey.
My name is Gary Crerie and along with Andrew Nguyen and Christine Baker we form the OWA RAP committee.
We hope as an organisation to have completed an Innovate RAP in the next two years
With your indulgence over future months we will provide some ongoing cultural awareness information that may help you in your practices and in your communities.
In this article we address:
- Why are we undertaking a RAP for the organisation?
- Reconciliation as an important step to equal access to health care
- What is Reconciliation?
- How does that relate to OWA and Optometrists?
Rural Health West - Visiting Optometrists Scheme
Outreach program funding announced – Current and prospective providers, please read the information below.
Rural Health West is pleased to advise that we have been awarded new agreements by the Australian Government Department of Health.
A four-year agreement has been received for Eye and Ear Surgical Support (EESS), Medical Outreach Indigenous Chronic Disease Program (MOICDP), Rural Health Outreach Fund (RHOF), and Visiting Optometrists Scheme (VOS) for the period 1 July 2020 to 30 June 2024.
Transition period 1 July 2020 – 31 December 2020
Due to the timing of receipt of contracts, Rural Health West will continue current services for a six-month transition period for EESS, MOICDP, RHOF and VOS (1 July 2020 to 31 December 2020). All current services in these programs have been reviewed by the Regional Services team and a Letter of Offer has been sent to service providers for the continuation of services for the six-month period.
Key upcoming milestones for EESS, MOICDP, RHOF and VOS
- Transition period: 1 July 2020 – 31 December 2020
- Funding round: Wednesday 5 August 2020 – Friday 28 August 2020
- Assessment and approvals: September 2020 – November 2020
- Outcome of funding round: December 2020
- New services commence: 1 January 2021
Open funding round
Rural Health West will be holding an open funding round from Wednesday 5 August 2020 to Friday 28 August 2020 12.00 pm (WST). During this period all current service providers and prospective service providers are required to submit applications for outreach services from 1 January 2021.
Applications will be submitted through an online portal. To request access to the portal, you must submit an online enquiry form. Access to the online portal will be available from the commencement of the funding round on Wednesday 5 August.
Applicants will be required to submit Service Application Forms for the period 1 January 2021 to 30 June 2024, with a Budget and Itinerary Form submitted for the period 1 January 2021 to 30 June 2021. Budgets for subsequent financial years will be reviewed as part of our annual review process.
It is anticipated that the funding round will be highly competitive, we therefore encourage applicants to collaborate with local stakeholders and work with communities to develop robust applications. Service proposals with evidence of community consultation and letters of support from local stakeholders are considered to be strong proposals.
More information regarding the open funding round and services from 1 January 2021 will be distributed prior to the funding round.
For all queries regarding the funding round, please contact the Regional Services team via email or phone (08) 6389 4500.
Visiting Optometrists Scheme
VOS aims to improve the eye health of people in regional, rural and remote locations by improving coordination and integration of new and existing eye health services and increasing access to optometry services.
For more information, please see the VOS Fact Sheet or Service Delivery Standards
Regional Services feedback survey 2017-2020
With the end of the 2017-2020 funding period, Rural Health West invites you to complete a quick survey about your experience as stakeholder involved in the delivery of services funded through the Australian Government Department of Health Outreach programs.
Completing this survey enables Rural Health West to collect information on the administration of the Outreach programs, identify and action any areas for improvement, and inform our reports to the Government.
Service Providers who are contracted through the Outreach program(s) will be sent a separate survey to provide their feedback.
If you would like more information regarding the survey, please contact the Regional Services team.
Complete the quick survey
Rheumatology and Optometry/Ophthalmology Working Together
Optometry has an opportunity to help our patients and work together more effectively with rheumatology and ophthalmology. DOWNLOAD DOCUMENT
This is about Plaquenil (and chloroquine) and communicating the results of screening and baseline tests for Bull’s eye maculopathy with rheumatology. Essentially, best practice suggests that full results should be communicated back to the patient and their rheumatologist.
Plaquenil is a very effective treatment for inflammatory and skin disorders with relatively few side effects compared to alternative treatments. However, after some years of use it can cause Bull’s eye maculopathy, a potentially debilitating visual loss.
Bull’s eye maculopathy is untreatable except for the cessation of Plaquenil use and even then the condition can progress from a relatively minor to a severe loss of visual function.
Baseline test should be performed within the first year of treatment and screenings at yearly intervals after five years of treatment unless there is an increased risk of toxicity, when more frequent screenings are indicated. Ideally, all data and an opinion should be included in the report to help the rheumatologist’s assessment and also assist with interpreting your report with other future reports, which may be generated elsewhere.
Members will of course use their discretion and clinical acumen but I would suggest the report include the Humphry Visual Field Analyser 30-2 (the 10-2 test is adequate in most cases but may fail with losses of a peri-central nature) test or Medmont central visual field test (with paracentral points added) and an assessment of posterior pole retinal thickness and retinal layer integrity with an SD-OCT.
Optometry and ophthalmology’s role in preventing Bull’s eye maculopathy is to alert rheumatology when there is any reasonable suspicion that Bull’s eye maculopathy may be possibly developing. I use the words reasonable and possibly because once the development of Bull’s eye maculopathy is certain the potentially insidious progression of this condition means it may be too late.
Bull’s eye maculopathy begins as a para-fixation (within 6° of fixation point) or peri-fixation (extending to 8°) loss of visual function characterised by damage to the outer retinal layers and retinal pigment epithelium. In most cases losses are para-central but in some cases and especially in Asian races the losses can be peri-central. As members know, the signs consist of subtle pigment hypo and hyper changes near the maculae but also possibly in the region of the arcades in peri-central loss with similar hypo and hyper fluorescent changes in auto-fluorescent imagery. Similarly, SD-OCT images show damage and thinning of the outer retinal layers.
As members know, the risk of Bull’s eye maculopathy developing is dependent on dose as a function of body weight, time taken and other factors, for example, such as impaired renal/liver function, tamoxifen use and pre-existing macula conditions.
The following charts indicate the risk of Bull’s eye maculopathy as a function of dose and time. For normal doses, less than 5mg/kg of body weight, risk is small within the first 5 years with the risk increasing with dose and time taken.
Rheumatology requests that we provide a full report when we screen patients for Bull’s eye maculopathy. The report should include visual field data and an SD-OCT assessment of retinal thickness and retinal layer integrity to provide a baseline and allow assessment of change, which may occur up to a decade or more into the future. Since clients may change location in this time frame a copy of the report should be sent to the client. Given that Rheumatologists (and/or other medical practitioners) may not be clear on the interpretation of these results, a summary of the findings may also assist in a patient’s management.
In cases where there is any suspicion of Bull’s eye maculopathy, it is recommended that referral to ophthalmology is initiated for an mf-ERG assessment of macular function. In WA this is performed at SCGH and for Medicare reasons needs to be arranged by the rheumatologist or ophthalmology.
For more information I suggest:
- Hydroxychloroquine and Chloroquine Retinopathy: Recommendations on Screening, Royal College of Ophthalmology 2018
- Recommendations on Screening for Chloroquine and Hydroxychloroquine Retinopathy (2016 Revision), American Academy of Ophthalmology Statement
- Melles RB, Marmor MF. The risk of toxic retinopathy in patients on long-term hydroxychloroquine therapy. JAMA Ophthalmol 2014;132:1453e60.2
- Xu P. Demystifying Bull’s Eye Maculopathy, Pharma, March 2020
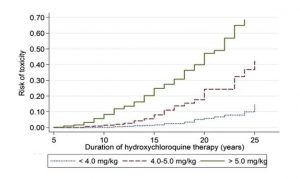
The cumulative risk of retinopathy over time, as a function of different levels of hydroxychloroquine (HCQ) use. When use is between 4.0 and 5.0 mg/kg, the risk is very low within the first 5 to 10 years, but it increases markedly afterwards. From: Melles RB, Marmor MF. The risk of toxic retinopathy in patients on long-term hydroxychloroquine therapy. JAMA Ophthalmol 2014;132:1453e60.2
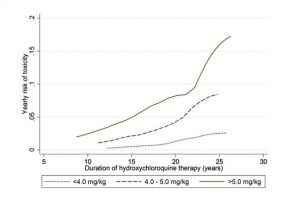
The incremental annual risk of toxicity for a patient at different levels of hydroxychloroquine (HCQ) use who is found to be free of retinopathy at a given point in time. The annual risk is low within the first 10 years of use, but increases with longer durations of therapy. From: Melles RB, Marmor MF. The risk of toxic retinopathy in patients on long-term hydroxychloroquine therapy. JAMA Ophthalmol 2014;132:1453e60.2





