1:30min
By Sandra Shaw
National Communications Manager
Despite reports that imaging technologies improve the stratification of AMD, this effect may be small when applied among practising optometrists without additional or specific training.
These were the findings of a study conducted by Angelica Ly, Dr Lisa Nivison-Smith, Dr Barbara Zangerl, Dr Nagi Assaad and Dr Michael Kalloniatis, and reported in their paper ‘Advanced imaging for the diagnosis of age-related macular degeneration: a case vignettes study’ published in Clinical and Experimental Optometry. READ with free access
The aim of the study was to evaluate the diagnosis, staging, imaging and management preferences, and the effect of advanced imaging among practising optometrists in age-related macular degeneration (AMD).
Up to 20 case vignettes, which were computer-based case simulations, were completed online in a computer laboratory in random order by 81 practising optometrists of Australia. Each case presented findings from a randomly selected patient seen previously at the Centre for Eye Health in Sydney for a macular assessment. Findings were presented in the following order: case history, preliminary tests and colour fundus photography.
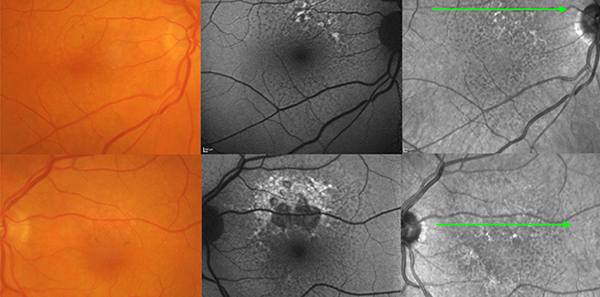
Participants were prompted to provide their diagnosis, management and imaging preference. One additional imaging result (variously, modified fundus photographs and infrared images, fundus autofluorescence, or optical coherence tomography [OCT]) was then provided and the questions repeated. Finally, all imaging results were provided and the questions repeated a third time.
A total of 1,436 responses were analysed. The presence of macular pathology in AMD was accurately detected in 94 per cent of instances. The overall diagnostic accuracy of AMD was 61 per cent using colour fundus photography. This improved by one per cent using one additional imaging modality and a further four per cent using all imaging.
Across all responses, a greater improvement in the diagnostic accuracy of AMD occurred following the presentation of OCT findings versus other modalities. OCT was the most preferred imaging modality for AMD, while multimodal imaging was of greatest benefit in cases more often misdiagnosed using colour fundus photography alone. Overall, the cohort also displayed a tendency to underestimate disease severity.
The authors say their data highlight that the effect of advanced imaging on diagnostic accuracy in AMD by a cohort of practising clinicians is small at five per cent and is associated with a higher intention to refer. The data also suggest an apparent lack of training among participants regarding the specific interpretation of imaging in AMD and provides unique insight into factors which may be useful for improving the current standard of care, they say.
‘The purpose of our study was to be descriptive rather than critical. Future studies are suggested in order to further highlight the commitment of eye-care professions to promote a high standard,’ the authors note.
‘Measurements of clinical practice, such as ours, may be used to evaluate and describe the current standard of eye-care, which may have clinico-legal implications; encourage confidence in the eye-care professions; determine future priorities in undergraduate or continuing postgraduate education and set a realistic groundwork for evidence-based practice and minimum standards of competency; and enable future measurements of the impact of change strategies.’
It was beyond the scope of the study to explore differences between groups of eye-care professionals based on their training or country of practice or to elucidate the specific reasons behind limitations in practice.